Breaking down the science of blood disorders: diagnosis and treatment
Blood disorders encompass a wide range of conditions that affect the components of our blood, including red blood cells, white blood cells, platelets, and plasma. These disorders can significantly impact our health and well-being, necessitating accurate diagnosis and effective treatment. Over the years, advances in medical science have shed light on the underlying mechanisms of various blood disorders, enabling healthcare professionals to make precise diagnoses and develop targeted therapies. In this article, we will delve into the science behind blood disorders, exploring the process of diagnosis and the latest treatment approaches.
Diagnosing blood disorders:
Accurate diagnosis is the foundation for effective treatment of blood disorders. Medical professionals employ various diagnostic techniques and tests to identify the specific type and severity of a blood disorder. Here are some common diagnostic methods:
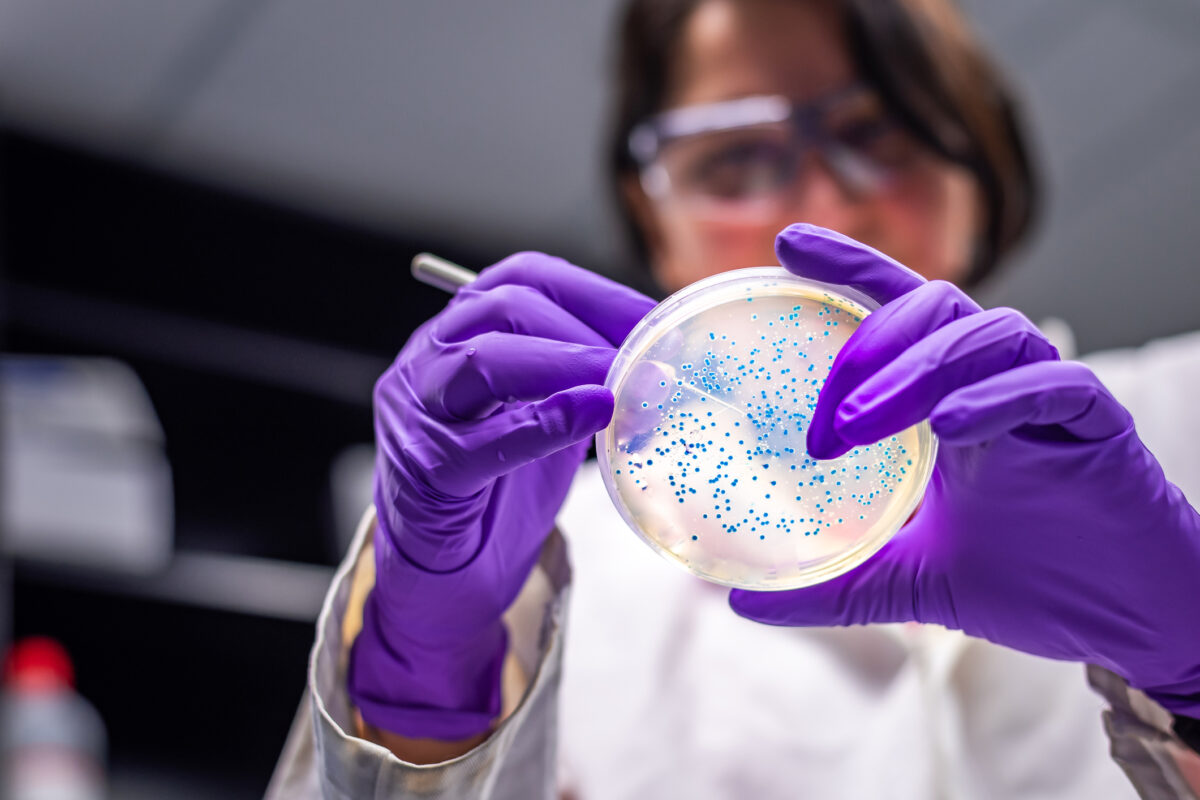
- Blood tests: Blood samples are analyzed to measure the levels of different blood components, such as red and white blood cells, platelets, and hemoglobin. Abnormalities in these levels can indicate the presence of a blood disorder.
- Bone marrow aspiration and biopsy: These procedures involve the collection and examination of bone marrow samples, which can reveal abnormalities in cell production or maturation. They are particularly useful in diagnosing disorders like leukemia or myelodysplastic syndromes.
- Genetic testing: Some blood disorders have a genetic basis. Genetic testing can identify specific gene mutations or abnormalities that contribute to the development of these disorders. This information can aid in diagnosis, prognosis, and even potential treatment options.
- Imaging studies: Imaging techniques like ultrasound, MRI, or CT scans can be utilized to evaluate the structure and function of organs involved in blood production and circulation. These tests can help identify any abnormalities that may contribute to blood disorders.
Understanding blood disorder treatment:
Once a blood disorder has been diagnosed, appropriate treatment strategies can be devised to manage the condition and improve the patient’s quality of life. Treatment plans are tailored to the specific disorder, its severity, and individual patient factors. Here are some common treatment approaches for blood disorders:
- Medications: Pharmacological interventions are often prescribed to manage blood disorders. For instance, patients with anemia may require iron supplements or erythropoietin-stimulating agents to increase red blood cell production. Anticoagulant medications may be administered to prevent blood clot formation in individuals with clotting disorders.
- Blood transfusions: In certain cases, blood transfusions may be necessary to replenish deficient blood components or improve their function. Transfusions of red blood cells, platelets, or clotting factors can be life-saving for patients with severe blood disorders.
- Stem cell transplantation: Stem cell transplantation, also known as bone marrow transplantation, is a potential treatment option for individuals with certain types of blood cancers or genetic blood disorders. Healthy stem cells are introduced into the patient’s body, replacing damaged or malfunctioning cells and restoring normal blood cell production.
- Gene therapy: With advancements in gene editing technologies, gene therapy is emerging as a promising approach for treating certain genetic blood disorders. This experimental technique aims to correct or modify faulty genes responsible for the disorder, offering the potential for long-term therapeutic benefits.
- Supportive care: Blood disorder treatments often require comprehensive supportive care measures. These may include dietary changes, lifestyle modifications, physical therapy, or psychological support to manage the symptoms and improve overall well-being.
The future of blood disorder management:
In recent years, scientific research has significantly contributed to our understanding of blood disorders and paved the way for innovative treatment approaches. Here are a few exciting developments on the horizon:
- Precision medicine: Advances in genomic analysis and personalized medicine hold tremendous promise for blood disorder management. Tailoring treatment plans based on an individual’s genetic profile can enhance efficacy and reduce adverse effects.
- Immunotherapies: Immunotherapies, such as monoclonal antibodies and chimeric antigen receptor (CAR) T-cell therapy, have shown remarkable success in treating certain types of blood cancers. These therapies harness the power of the immune system to target and destroy cancer cells specifically.
- Gene editing techniques: The development of precise gene editing tools like CRISPR-Cas9 has opened up new avenues for correcting genetic defects responsible for blood disorders. Ongoing research in this field holds the potential for curative treatments.
- Stem cell research: Scientists continue to explore the therapeutic potential of stem cells for blood disorder treatment. Understanding the mechanisms governing stem cell behavior and differentiation can lead to innovative therapies and regenerative medicine approaches.
The science behind blood disorders has come a long way, empowering healthcare professionals to diagnose these conditions accurately and devise effective treatment plans. With ongoing advancements in diagnostics, pharmacology, genetic research, and innovative therapies, the future looks promising for individuals with blood disorders. Collaborative efforts between researchers, clinicians, and patients are vital to further unravel the complexities of these disorders and develop improved strategies for diagnosis and treatment, ultimately improving outcomes and enhancing the quality of life for those affected by blood disorders.